
February 2020
Positive Effect of Collaborative Chronic Care Model on VA Mental HealthThe Chronic Care Model includes several – or all - of the following elements: work role redesign to support continuous care; patient self-management support; provider decision support; clinical information systems; linkage to community resources; and healthcare leadership support. These elements should be flexibly implemented depending on local needs, capabilities, and priorities. Takeaway: A partnership between QUERI, VA’s Office of Mental Health and Suicide Prevention, and the Office of Veterans Access to Care resulted in the implementation of a Collaborative Chronic Care Model that incorporated Behavioral Health Interdisciplinary Program teams to treat Veterans with mental health conditions. This intervention led to significantly decreased mental health hospitalizations for Veterans and has been spread to 21 additional VA healthcare facilities. Mental health conditions affect 47% of Americans during their lives and impact 27% in any given year. Outcomes for individuals with mental health conditions is suboptimal, and care coordination is problematic, even in integrated healthcare systems such as VA. Multicomponent care models that emphasize care coordination and evidence-based care have been shown to improve health outcomes for individuals across a variety of medical conditions. Specifically, the Chronic Care Model was developed for chronic medical illnesses treated in primary care. This article describes a multistage effort by QUERI investigators that evolved over eight years to move the Collaborative Chronic Care Model (CCM) – an adaptation of the Chronic Care Model – into broad use for Veterans with mental health conditions treated in the VA healthcare system.1 This eight-year journey started with an evidence synthesis that was conducted beginning in 2010, when QUERI and HSR&D investigators compiled data on randomized controlled trials of CCMs for any mental health condition. This systematic review demonstrated the effectiveness of CCM across mental health conditions (i.e., depression, bipolar disorder, and anxiety disorders) for individuals treated in mental health clinics as well as primary care settings. 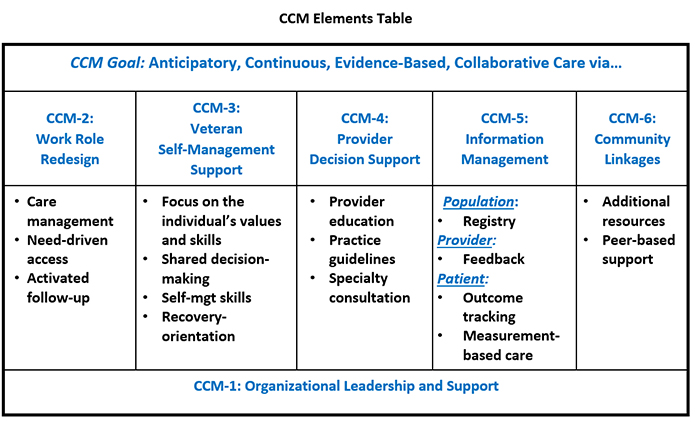
Policy Impact In 2013, VA’s Office of Mental Health and Suicide Prevention (OMHSP) began a high-priority effort to enhance care coordination in general mental health clinics by establishing interdisciplinary teams (called Behavioral Health Interdisciplinary Program, or BHIP, teams) in each VA medical center nationally. OMHSP had disseminated centralized guidance via multiple communication and educational methods, though facilities were given broad latitude to develop team processes locally. OMHSP then became aware of the evidence synthesis, and in 2015 adopted the CCM as the model for their outpatient mental health teams. In addition, OMHSP collaborated with study investigators to develop CCM training materials and implementation support methods to augment pre-existing BHIP guidance. Implementation Trial From February 2016 through February 2018, QUERI investigators again partnered with OMHSP to conduct one of the first studies to evaluate CCM implementation for individuals treated in mental health clinics.2 Funded through QUERI, this randomized implementation trial established CCM-based teams in nine outpatient general mental health clinics. The study included 5,596 Veterans treated in mental health clinic BHIP teams (excluding Veterans with dementia) and 62 VA providers on those BHIP teams. CCM implementation support focused on facilitating local solutions for local challenges that could be developed with evidence-based guidance, which required team-building and attention to healthcare processes. Implementation activities led teams through self-assessment and process improvement efforts to align clinical processes with the CCM elements (leadership support, work role redesign, Veteran self-management, provider decision support, information management, and community linkages). Implementation outcomes focused on team function (communication, cohesion, role clarity, and team primacy) and concordance with the six CCM elements. Intervention outcomes included Veteran health status data, which were gathered during telephone interviews at baseline, 6, and 12 months of implementation support and via VA Corporate Data Warehouse data. Implementation Trial Findings
Further, this implementation initiative used existing clinical staff, with external facilitation the only added research-supported effort, totaling less than three hours per week per facility, and still decreased hospitalization rates and, for complex individuals, improved mental health status. This experience highlights the synergy possible among research, policymaking, program development, and implementation – and the benefits of working within a learning health care system. Learning Healthcare System This multiyear process included a comprehensive evidence synthesis that provided leverage for evidence-based change for VA mental health services – and stimulated a partnership between health system leadership and implementation researchers. The partnership then collaborated to design and conduct a formal implementation trial that was guided by the evidence synthesis. Subsequently, with strong buy-in from the health system leadership of OMHSP and the Office of Veterans Access to Care, a scale-up and spread effort supported by the evidence synthesis was conducted, extending implementation facilitations to 21 more VA medical centers.1 This experience highlights the synergy possible among research, policymaking, program development, and implementation – and the benefits of working within a learning health care system. For more information about this research, please contact Mark Bauer, MD, part of the Team-Based Behavioral Health QUERI National Program and HSR&D’s Center for Healthcare Organization and Implementation Research (CHOIR) at Mark.Bauer@va.gov . References
|